A Scientific Guide to Chronic Gastritis Treatment in China: Winning the Battle for Your Stomach's Health
- MedBridge NZ
- Oct 2, 2025
- 4 min read
Updated: Feb 21
Key Takeaways
Targeted Eradication: Chronic gastritis is predominantly driven by H. pylori infections; utilizing targeted quadruple therapy is crucial for effective reversal.
Proactive Monitoring: If left unchecked, conditions like atrophic gastritis can advance to precancerous states (intestinal metaplasia), requiring strict endoscopic surveillance.
Seamless Access to Top Care: MedBridgeNZ facilitates expedited access to leading Chinese gastroenterologists, handling all logistical and language barriers for international patients seeking chronic gastritis treatment in China.
Chronic gastritis is one of the most common stomach ailments, a condition that many of us will encounter at some point in our lives. It acts as a silent alarm, initially presenting with mild symptoms like upper abdominal pain or bloating. However, if left unaddressed, it can lead to more severe health issues. This article will provide a scientific overview of chronic gastritis and guide you on how to manage it effectively.
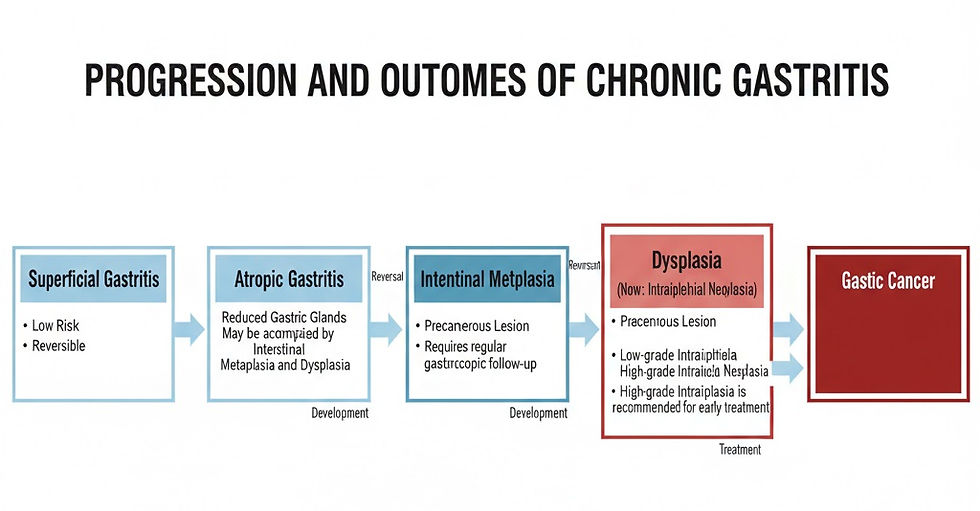
Chronic Gastritis: A Persistent Battle in Your Stomach Lining
The Mechanism: An Imbalance of Damage and Repair
The gastric mucosa is the natural barrier that protects your stomach wall. When factors such as Helicobacter pylori (H. pylori) infection, long-term medication use, or bile reflux repeatedly attack this lining, the stomach's self-repair capabilities can become overwhelmed, leading to chronic inflammation.
Key Causes:
Helicobacter pylori (H. pylori) Infection: Approximately 70% of chronic gastritis cases are linked to this bacterium, which embeds itself in the stomach lining and releases toxins that cause inflammation.
Medication-Induced Damage: Long-term use of drugs like aspirin and ibuprofen can weaken the protective mechanisms of the gastric mucosa.
Unhealthy Lifestyle Habits: Excessive alcohol consumption, smoking, a high-salt diet, and high levels of stress can all exacerbate damage to the stomach lining.
Superficial vs. Atrophic Gastritis: Understanding the Depth of Inflammation
Chronic gastritis is classified into two types based on the severity of the condition, each with different risks and management strategies:
Superficial Gastritis: Inflammation is confined to the surface layer of the gastric mucosa. This is a low-risk, reversible condition.
Atrophic Gastritis: Characterized by a reduction in gastric glands and a thinning of the mucosal layer. This condition carries a higher risk of developing into cancer and requires careful monitoring.
While symptoms for both can be similar (e.g., upper abdominal discomfort, belching), atrophic gastritis may also be accompanied by a loss of appetite and anemia due to reduced iron absorption from decreased stomach acid. It is important to note that "atrophic gastritis" refers to a reduction in glands, not a "shrinking stomach," and timely intervention can slow its progression.
Intestinal Metaplasia & Intraepithelial Neoplasia: The Warning Signs
When the gastric mucosa is damaged over a long period, some cells may transform into intestinal-like epithelial cells, a condition known as intestinal metaplasia. This is a precancerous state, and while it doesn't mean you have cancer, it requires regular monitoring through gastroscopy.
Intraepithelial neoplasia (previously known as dysplasia) refers to abnormal structural changes in the cells of the gastric mucosa. High-grade neoplasia is considered a precancerous lesion and requires immediate treatment, often through endoscopic resection or surgery.
Treatment Principles: Addressing the Root Cause
The treatment of chronic gastritis requires a comprehensive medical approach:
Eradicate H. pylori (Crucial!): The standard treatment is a "quadruple therapy" regimen, which includes a proton pump inhibitor, two antibiotics, and a bismuth agent, for a course of 10-14 days. Eradicating H. pylori can, in some cases, reverse intestinal metaplasia.
Protect the Gastric Mucosa: Specific medications can help repair the stomach lining.
Lifestyle Adjustments: Eat smaller, more frequent meals, avoid pickled, fried, and overly hot foods, quit smoking, limit alcohol, and manage stress.
For international patients seeking these advanced treatments, navigating a foreign healthcare system can be daunting. A dedicated medical concierge provider can assist in coordinating fast-tracked appointments, managing travel logistics, and providing medical translation, ensuring a seamless healthcare experience in China.
Gastroscopy Follow-Up: Keeping Risks in Check
Regular monitoring is key to managing chronic gastritis:
Atrophic Gastritis (without intestinal metaplasia or neoplasia): Every 2-3 years.
Atrophic Gastritis with Intestinal Metaplasia: Every 1-2 years.
Low-Grade Intraepithelial Neoplasia: Every 6-12 months.
High-Grade Intraepithelial Neoplasia: Immediate treatment.
Conclusion
Chronic gastritis is a health reminder from your body. Through proactive management, including eradicating H. pylori, regular follow-ups, and lifestyle adjustments, you can effectively control the risks. Remember, the well-being of your stomach is in your hands.
Medical content reviewed and authored by Dr. Chen Li, Chief Physician, Department of Gastroenterology at Shanghai Ruijin Hospital.
Ready to Consult a Top Gastroenterologist in China? Navigating cross-border healthcare shouldn't be as stressful as the condition itself. At MedBridgeNZ, we specialize in bridging the gap between international patients and China's leading medical experts. While we do not provide medical advice ourselves, our concierge team will handle your hospital appointments, medical record translations, and travel logistics, ensuring you have direct access to experts like Dr. Chen Li.
[Contact the MedBridgeNZ Team Today] to discuss your medical travel needs and let us facilitate your journey to better health.



